Author(s): Yusuf Ismail
Originally published on Towards AI.
Think about this.
It is 2 o’clock in the night. You are on a trolley in a hospital corridor. Not ward. an aisle. Fluorescent lights, the smell of disinfectant, the sound of a ward that’s packed somewhere behind a set of doors that just won’t open for you.
A doctor saw you three hours ago. He decided that you needed to enlist. She wrote it down, made the call, and moved on to the next patient. The bed he ordered for you doesn’t exist yet. So you wait. On the trolley. In the corridor. While the clock runs.
This is not the worst situation. It is Tuesday.
I’ve been building data pipelines on NHS performance data for the last few months: outpatient records, referral-to-treatment waiting times, and now A&E. The deeper I dig into this data, the more I realize that what I’m seeing is not a pressurized system. It is a system that has quietly normalized something that should never have been normal.
1,280 patients. Every day. Stuck in the corridors because the doctor had already decided he needed a bed.
I wanted to see that number. So I made something to track this properly.
the target no one is touching
The NHS has one goal. This is from 2000. 95% of patients attending A&E must be seen, treated and either admitted, discharged or transferred within four hours of arrival.
Quite simple. Measurable. Published monthly by NHS England for anyone to download.
So I downloaded it. All this. 36 months. April 2022 to March 2025. Every NHS Trust in England, every month, submits their numbers in CSV files to a government website, which most people will never visit.
I built a Bronze→Silver→Gold medal pipeline in Python – ingesting raw files, cleaning and classifying them, then calculating those important metrics. 36 files. 7,238 rows of provider-level data after the transformation. The three gold tables: national, regional, trust-level.
Then I ran the numbers.
0 out of 36 months achieved 95% target. Not one. not even close.
The best month in three years was April 2023 – 65.5%. The worst was December 2023 – 54.3%. The average over the entire period was 59.8%. The NHS is on average 35 percentage points below its target. Every single month.
19.5 million people waited more than four hours in major A&E between April 2022 and March 2025. That’s 19.5 million moments when someone sat in pain, or fear, or exhaustion, after the system promised they wouldn’t have to.

corridor care number
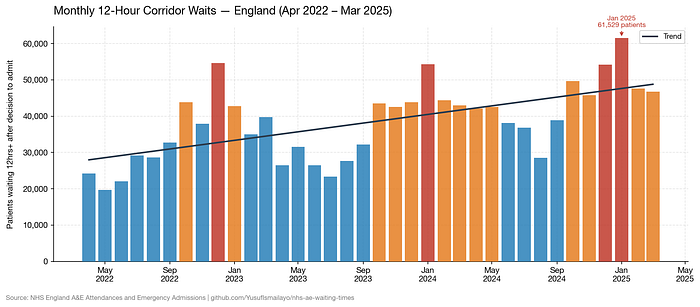
Beneath the four-hour headline is a number that doesn’t get enough attention – the 12-hour wait. There are no 12 hours to watch. After 12 hours the doctor has decided that you need to be admitted. You are in the corridor. The system can’t find anywhere to place you.
1,381,891 people experienced it in three years. And it seems to be getting worse:
2022/23: 410,029 corridor waits of 12 hours or more
2023/24: 439,411
2024/25: 532,451
This is an increase of 30% in three years. December is consistently the worst month – an average of 50,879 people wait 12 hours or more each December. Winter is no surprise. This happens every year. The system knows it’s coming.
your postcode is variable
I was on a call with my evaluator earlier this year. Somewhere in the conversation, I mentioned what I was building – NHS pipelines, waiting time data, postcode lottery searches emerging from the numbers.
She stopped. Then she told me where she lived in rural Wales. If she calls her GP in the morning, she is seen the same day. Her father, who lives in England, has to go online, fill out a form, and hope the algorithm decides it’s urgent enough.
He told me about the ambulance. Wherever she lives, they come. In England, he said, the first thing they ask you is if you’re breathing — because the triage system is under so much pressure that the questions you answer over the phone determine whether help will come. He noted the delay in care for his father during a serious health episode. I did not investigate further.
He mentioned that once, in his part of Wales, the coastguard arrived when he called for an ambulance. Because he can reach there first.
I went back to my data.
Because what he described – that difference, the difference in what the system gives you depending on where you live – is exactly what the numbers show.
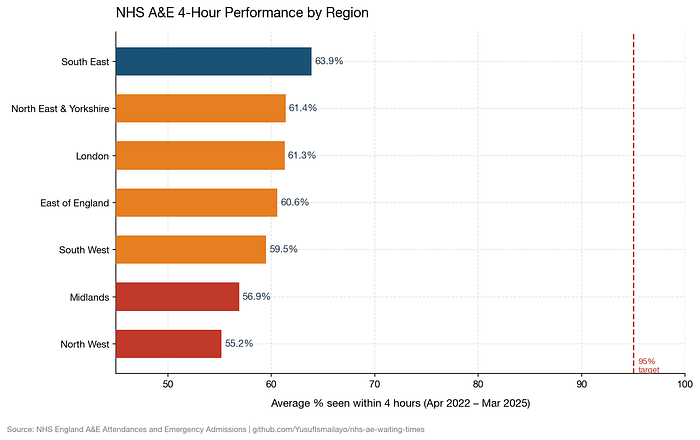
The best performing region in England over the three years is the South East, averaging 63.9%. The North West is the worst with 55.2%. But regional differences are nothing compared to trust-level differences.
Best performing major A&E trust: Sheffield Children’s NHS Foundation Trust – 90.2% average.
Worst: United Lincolnshire Hospitals NHS Trust – 40.5%.
49.7 percent marks between them. Same country. Same goal. Same NHS. Different postcode.
which hit different
I live in Telford.
When I pulled the trust-level data and sorted it, I wasn’t looking for anything specific. I was just reading the list of worst performers.
Was there.
Shrewsbury and Telford Hospitals NHS Trust. Third worst in England. 43.6% average four-hour performance over 36 months. 825 patients per month are waiting 12 hours or more after an admission decision.
This is the hospital that serves the city I live in.
If anything goes wrong tonight my family will go to A&E.
43.6%.
I don’t say this to attack the employees. Anyone who has worked in or around the NHS knows that the people there are doing everything they can. But data is data. And the data says that if you live in Telford and you go to A&E, less than half of the patients are being seen within the target time. Every month. Continuous. for three years.
It’s not a bad week. That’s the baseline.
What the data really says
This is what three years of NHS A&E data tells us:
The system is not working properly. Every region of England performed worse in 2023/24 than in 2022/23. Most remained slightly stable in 2024/25 but never improved the situation. North West has been below 56% for three consecutive years. The Midlands has accumulated 314,606 twelve-hour corridor waits since April 2022.
The 95% target was last met at the national level in 2015. This was a decade ago.
48 million people in England attended a major A&E between April 2022 and March 2025. About 20 million of them waited longer than they should have. 1.38 million were left in the corridors because a doctor had already decided they needed care.
And if you want to know if you’re likely to be one of them, the most reliable predictor isn’t how sick you are. This is where you live.
line pipe
The full code is on GitHub – bronze ingestion, silver transformation, gold analytical tables. Every number in this article comes directly from published data from NHS England, processed through a reproducible pipeline that anyone can clone and run.
GitHub: https://github.com/YusufIsmailayo/nhs-ae-waiting-times
to close
My evaluator ended that part of our conversation by saying something I keep returning to.
She said: Where you live should not determine how much care you get.
He said it casually, as if it was obvious. As if it was something everyone already knew.
Maybe they do. Maybe this is the problem. We know it. We have known this for years. The data is published every month. The target is missed every month. And even at 2 o’clock in the night the corridor is full.
Today 1,280 people. Stuck. waiting. After the decision has already been made.
I created a pipeline to measure this. I’m not sure that’s enough. But it seemed necessary to count.
Yusuf Ismail is a data engineer building NHS analytics pipelines. Their previous projects include 226 million outpatient records and 14 million RTT pathways. GitHub: Yusuf Ismailayo | medium: @yusufismail_91982
Published via Towards AI

