Unlock Editor’s Digest for free
FT editor Roula Khalaf selects her favorite stories in this weekly newspaper.
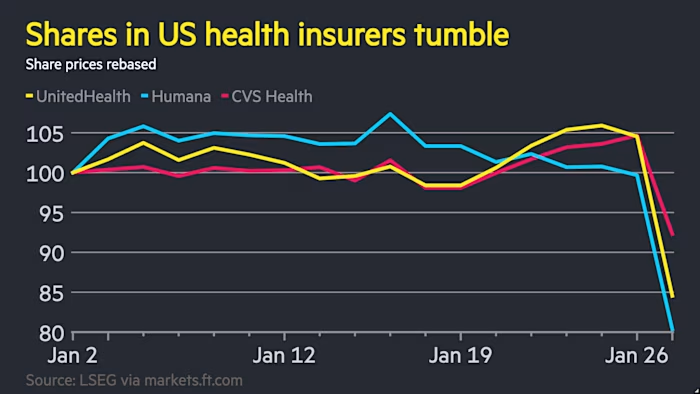
US health insurance stocks fell on Tuesday after the Trump administration said it would reduce spending on a popular government-funded plan for older Americans.
UnitedHealth and Humana, the largest providers of government-subsidized insurance plans known as Medicare Advantage plans, lost about a fifth of their market value on Tuesday.
The defeat comes as the Centers for Medicare & Medicaid Services said late Monday that it planned to increase some 2027 payments to companies providing coverage for seniors and people with disabilities by just 0.09 percent — or about $700 million. CMS had approved a 5 percent rate increase for insurance companies for 2026.
The CMS proposal is the latest in recent weeks that the Trump administration has shocked markets with its policy plans. Earlier this month, a plan to block institutional investors from buying single-family homes rocked shares of big landlords, while many bankers objected to the president’s call to cap credit card interest rates.
Medicare Advantage is attractive to the insurance industry: According to a congressional report, insurers were expected to be paid about $540 billion by the U.S. government in 2025 to run subsidized insurance plans.
“Insurers are facing a difficult political environment, which is unusual for a Republican regime,” Oppenheimer analysts said. “Inflation has been running above historical levels for several years and the (Medicare) rate update significantly bucks that trend.”
Humana shares were down 20 percent in afternoon trading in New York, while UnitedHealth was down 19 percent. Aetna owner CVS Health declined 13 percent, while analysts warned that the rate is just a proposal and could rise before it is finalized in April.
CMS’s announcement created more problems for UnitedHealth, which reported financial results on Tuesday. The Minneapolis-based company warned that revenue would fall for the first time in at least three decades.
UnitedHealth, which provided coverage to 9.9 million people on Advantage plans last year, is particularly exposed to some plans within Medicare, according to KFF, a nonprofit health policy research group. The Medicare Advantage healthcare plan, a privately managed alternative to traditional government-administered healthcare, provides coverage for more than 34 million elderly Americans and people with disabilities.
“While UnitedHealth’s recovery story remains volatile, CMS’s recent announcement complicates the long-term recovery story for UnitedHealth and the industry as a whole,” JPMorgan analysts said.
In a call with analysts Tuesday, UnitedHealth executive Tim Noel acknowledged that CMS’s announcement was “disappointing.” The company’s shares have fallen by 47 percent in the last 12 months.
Last May, the company ousted Chief Executive Andrew Witty and brought back its longtime CEO Stephen Hemsley in a bid to revive its fortunes.
It also acknowledged a Justice Department criminal investigation related to its Medicare billing program. In December 2024, company executive Brian Thompson was shot and killed in a targeted killing. Suspect Luigi Mangione is expected to stand trial later this year.
UnitedHealth also reported that its profits fell 41 per cent to $19bn last year after its bottom line was hit by $1.6bn in restructuring costs linked to the cyberattack.
“As the narrative becomes more complex, we are becoming increasingly concerned about UnitedHealth’s fundamental story,” Baird analysts wrote Tuesday. “Why is UnitedHealth suddenly filing a cyberattack allegation again in the fourth quarter (of 2025)?”